Diagnosing Keratoconus
- Details
- Published: Wednesday, 21 October 2015 08:28
- Written by Keratoconus Academy
With new technologies that measure the shape and thickness of the cornea in exquisite detail, we are now able to detect the presence of keratoconus well before subjective symptoms develop. Corneal Topography has become the standard of care in diagnosing keratoconus. A computerized system images the shape of the cornea by taking tens of thousands of data points from the corneal surface. The results are instantly analyzed and a topography map is generated. The colors of the map correspond to the shape of the cornea. In keratoconus the cornea tends to be very steep in shape and quite irregular in shape. Quantitatively the topography values can be monitored for change over time to determine if the condition is progressive.
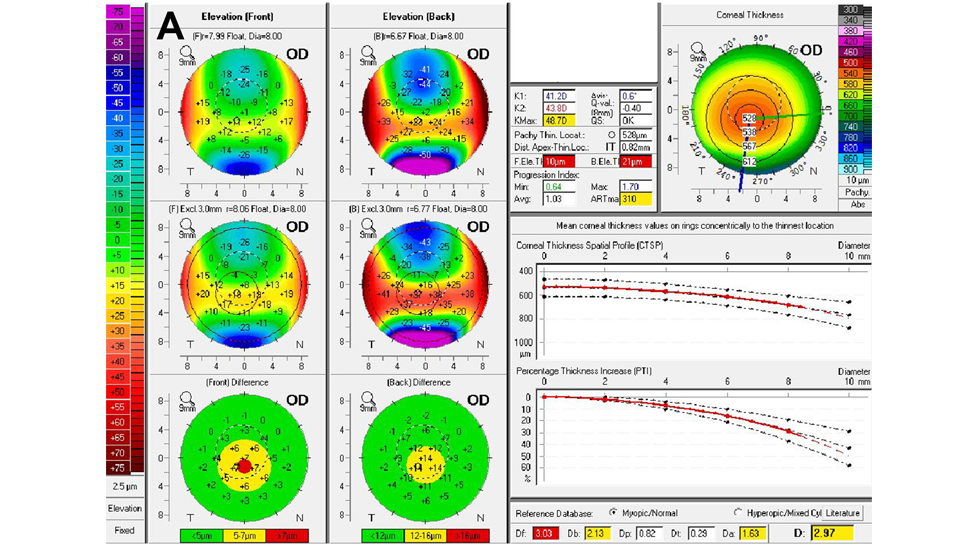
Tomographic corneal analysis (examples are Pentacam, Orbscan and Galilei systems) differs from other topography systems in that it not only measures the front surface of the cornea, but it also measures the back surface of the cornea, the thickness of the entire cornea (global pachymetry), and images and analyzes the anterior ocular structures as well. This is very critical in keratoconus since we have discovered that the back surface of the cornea is affected earlier and to a greater degree than the front corneal surface is in keratoconus. Thickness variations from normal are also early hints in terms of the presence of keratoconus and in the determination of progression in keratoconus. Additionally, software programs have been developed, such as the Belin Abrosio Ectasia Display available for Pentacam, that statistically analyze various elements measured by tomography that would suggest the presence of corneal ectasia.
Early phases of keratoconus will typically have abnormalities found with tomography and topography, yet have no other detectable clinical signs or subjective patient symptoms. As keratoconus develops and progresses, clinical signs and subjective symptoms will eventually show up. At some point in the disease process your doctor will note visible thinning of the cornea under the biomicroscope along with folds in the cornea (called "striae"). Other clinical signs include the deposition of iron in the cornea ("Fleisher's Rings"), corneal scares, large increases in astigmatism, and reduced correctable vision with glasses. Patients complain of distortion and progressive blur of their vision along with large and frequent changes in their prescription. Today with the advent of treatments that can slow down if not halt the progression of keratoconus - it has become critically important to diagnose the disease as early as possible.
Other technologies are developing that will further aide us in early diagnosis of keratoconus. Anterior segment optical coherence tomography (ASOCT) systems are developing analytic software for their pachymentric measurements that will detect early changes in corneal thickness, especially thickness progression changes from corneal center to periphery. Additionally, ASOCT systems are developing methods to measure and analyze corneal epithelial thickness. Studies are showing that apical corneal epithelial thinning and paracentral thickening may be some of the earliest signs of the development of keratoconus. Corneal biomechanics are also thought to be a measurement that will show very early changes as keratoconus develops. Systems that measure the biomechanical properties of the cornea may enable the eye care practitioner to discover abnormalities far earlier in the disease development and surely before clinical signs show up that effect vision. Thus again, enabling us to intervene early to prevent progression to a clinically significant state.